
It is a common problem. Every year, hospitals lose millions of dollars when items used in the course of a patient’s care somehow slip through the system without ever being charged or reimbursed. At Yale-New Haven Hospital in Connecticut, a Six Sigma project team decided to look at the opportunities related to patient charge capture. The first thing the team realized was the importance of scoping this project to set realistic parameters.
Patient charge capture is a complex area. Others had tried to tackle it without much success because of the overwhelming number of items that could potentially come under review. To make the effort more manageable, the team at Yale-New Haven decided to focus on the top 12 supplies based on quantity and expense, and limit the project to seven pilot units. The team assumed that if it could fix the process for those 12 items, chances were other items would benefit from the changes as well.
As the team began to collect and review the data associated with the selected items, it made some surprising discoveries:
- About 36 percent (35.7) of patient charge items (medical/surgical supplies) were being captured in inpatient nursing units. This was based on an analysis of fiscal year 2003.
- For the top 12 supplies used there was an opportunity to increase gross charges by an estimated $4.5 million.
- In inpatient units, there was no standard method of processing patient charge items.
With the Big Y identified as patient charge capture, the team identified a series of manageable sub-Ys or sub-cycles to focus on. The process map the team created contained so many different, interconnected steps that it seemed difficult to believe that anything could be properly charged.
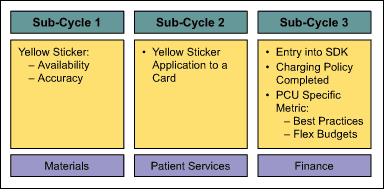
The process was divided into three sub-cycles:
About Yale-New Haven Hospital
- Founded in 1826
- A 944-bed private, not-for-profit teaching hospital
- Affiliated with the Yale University schools of medicine and nursing
- Approximately 6,000 employees, including 1,200 registered nurses and a medical staff of more than 3,000
- About 47,000 inpatients annually, and more than 462,057 outpatient visits each year
In an effort to reduce errors and increase efficiency, there is often a tendency in healthcare to immediately reach for a technology solution. In the case of charge capture, many dispensing devices exist that could potentially assist in maintaining inventory and billing patients. But such technologies are expensive, and there is no guaranteed return on investment. Also, introducing new technologies without a solid process in place could cause more problems. Instead of automating a broken system, the team decided the first step was to fix the broken process.
Some of the stakeholders wanted to first focus on sub-cycle 1, making sure all the products that were supposed to have yellow stickers had a sticker and the correct one. This was in response to an audit indicating that as many as 10 percent of the products received from vendors that were supposed to be stickered were not and that a handful of products had stickers with inaccurate codes that could not be billed. Other stakeholders wanted to focus on sub-cycle 2, making sure that every chargeable item used in a patient care unit had its yellow sticker removed and affixed to a charge card with the five required patient demographic elements necessary for billing. The sponsors decided to focus on this second sub-cycle first since all the stakeholders were internal to Yale-New Haven Hospital, and theoretically would have greater control over solution identification and implementation. Sub-cycle 1, which was more complex because it had both internal and external stakeholders, would be the second issue addressed.
Sub-Cycle 2: Sticker Application to Patient’s Charge Card
One of the sub-Ys addressed the goal of improving documentation of the five required data elements on the charge cards. The team believed this could:
- Reduce cycle time from use of product to charging of product.
- Reduce defects such as cards that cannot be billed.
- Reduce re-work associated with obtaining required data elements manually.
As part of the effort to improve sub-cycle 2, the staff received training on new procedures and written manuals for reference. Previously, everyone had received training on the process through word of mouth.
An initial Work-out session was conducted to streamline and simplify sticker application to a patient charge card. The result was a simplified middle process – steps were removed, opportunities for defects were eliminated, the process was standardized and documented.
Sub-Cycle 1: Items Without Stickers
The team’s investigation of the items which arrived in totes from vendors without stickers indicated that the most common reasons were auto-substitution and back-ordered items. The team also found that in some cases, the outer packaging had yellow charge stickers, but the individual products inside did not. Each of these three missing sticker factors varied from the typical stickering process and therefore would require its own standard operating procedure to insure sticker placement on chargeable products.
The team held two separate Work-out sessions to streamline and simplify some of the process steps, making sure stickers were on products when they were delivered to the units. The results of the second session for the sub-cycle 1 is summarized in three solutions:
- Improve the pick process
- Develop an accurate list of patient charge items
- Improve communication systems
| Table 1: Details of Sub-Cycle 1 Solutions | ||
| Pick Process | Accurate List of Items | Communication Systems |
|
|
|
Changing the System
Applying Six Sigma and change management tools, the team was able to eliminate some of the unnecessary steps in the patient charge capture process. Fewer steps and handoffs meant the team also was able to eliminate some opportunities for defects.
The charge card was redesigned so that the five required data elements would automatically print out. To minimize confusion, the team had the cards placed in highly visible places, and always in the same place in every care unit.
The team also developed a unit report to reconcile differences between what each unit was purchasing and what each was charging out to patients. One unit may borrow supplies from another unit, which can throw off the tracking system. For instance, an ICU may purchase multiple kits that do not necessarily make sense for the entire floor to stock, so people tend to borrow the items when needed.
Another reason for tackling this project was to address the need for a better cost accounting system to improve managed care negotiations. The process changes were useful in this regard.
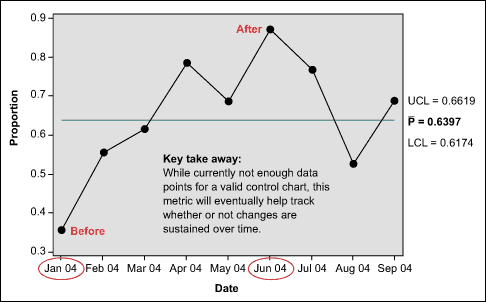
With improvements in place, the following control chart was developed to make sure results are maintained:
Results and Next Steps
By all measures, this project at Yale-New Haven Hospital was very successful. The changes the team was able to implement delivered statistically significant results. Within the seven pilot units, the team was able to move from capturing 35.7 percent of patient charges to 87.5 percent captured. With the project in the control phase, the hospital is continuing to monitor the indicators to make sure the units stay on track.
For the 12 products on the seven pilot units, the hospital was able to capture $197,000 more in gross charges than they would have at the January charge capture rates. On an annualized basis, this equates to an estimated $600,000 for seven pilot units and 12 items. For all 34 inpatient units, the annualized gross revenue for the 12 items amounts to an estimated $3.0 million. Assuming net revenue at 10 pecent of gross, then net revenue is $300,000. The team anticipates that the actual financial benefits will be significantly higher once a reliable accounting system is in place to accurately capture all charge items.
There are other benefits from the project as well. The hospital team is starting to capture the information by patients in the database. Having numerous patient charges missing from the system made it appear the hospital was actually using fewer products per case. This caused the hospital to underestimate the amount spent on each diagnosis related group (DRG).
With the project completed and improvements in place, the hospital is now able to better reflect the actual cost of caring for patients. Looking ahead to next steps in improving the charge capture process, the hospital is preparing to launch projects that will target whether or not the charges actually end up on the patient’s bill.