
Competition in the outpatient imaging center market is intense. New imaging centers are springing up everywhere. Faced with decreasing reimbursements, ever-changing technology and the expectation of spa-like atmospheres, how can an outpatient imaging center remain profitable? The answer lies with the customer.
Having a pulse on the customer experience and continually eliciting and acting on customer feedback is the way to win. If physicians and patients are happy with the service they receive, they will come back. One northern California hospital that operates multiple imaging centers created a program to listen to their customer feedback and develop a roadmap for improvement.
The hospital began its efforts at an outpatient facility in the San Francisco Bay Area, California. With three competitors located within 10 miles, this facility’s management knew it had to act quickly to gain customer loyalty. To learn about their strengths and weaknesses, the technologists headed out to the lobby to chat with patients, the medical assistants talked to the physician office managers, and the radiologists talked to referring physicians.
A laundry list of improvement ideas was forming, but one central theme was voiced repeatedly – decrease report turnaround time (TAT). Physicians wanted to be able to diagnose their patients sooner; and patients wanted to know the status of their health as soon as possible.
The objective was clear, but how to get there was not as evident. The center’s leadership decided to utilize the Six Sigma toolkit and the DMAIC (Define, Measure, Analyze, Improve, Control) process to determine the root causes for current turnaround times. Data would pinpoint the necessary improvements and drive management decisions.
Define and Measure Phases of Project
During the Define phase, project team members were identified, a project goal was agreed upon and all of the steps in the report turnaround process were mapped (Figure 1). The common industry standard at the time of the project was a 24-hour turnaround, so the team set its sights on meeting or exceeding that standard. As the team took a step back and observed the process, it realized that issues from scheduling all the way to report delivery were having an impact on the report TAT. But team members also determined that some process steps were under their control (as indicated by the red box in Figure 1). The team could make rapid changes to these steps without affecting other departments.
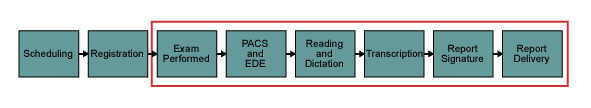
With the goal set (a 24-hour turnaround), the team’s next step was to determine the starting point. Data was collected and the current average turnaround at the center was calculated to be 64 hours – many hours away from the goal.
Analyze and Improve Phases of Project
Statistical analysis of the process data showed that four key steps were adding a considerable amount of time to the turnaround:
- Technician data entry into the radiology information system (RIS)
- Transcription
- Report signature
- Report delivery
When technicians completed scans, they pushed the images to PACS (picture archiving and communications system) but often forgot to close out the exam in the RIS. The problem with missing this step was twofold: 1) the report could not be sent out and 2) the facility would not be reimbursed. The technicians did not fully understand the importance of the step and therefore they discounted it. Through RIS training and process education, the team highlighted the importance of the step and began to see a change in behavior. To help sustain the progress, a report was developed to highlight missing RIS data. With the report, defects can be identified quickly and fixed in a timely manner.
The transition from dictation to transcription to signature was causing reports to sit for hours. The transcription team was overloaded and took scans on a first-come-first-served basis. When transcription was complete, the report went back to the radiologist for signature. Then radiologists had to re-familiarize themselves with the case before signing off. There were long wait times at every transition in the process. With strong support from the chief radiologist, the facility implemented new software so radiologists could dictate, verify and sign off on reports within minutes, thus eliminating transcription.
As with any new process, there were growing pains (Figure 2). The early adopters had to learn the new software, work with the voice recognition, and sell the new process to their fellow radiologists. Even though this was a difficult transition, the impact on report wait time was significant.

When the new software for radiologists was implemented, the final issue became evident. Reports were signed and ready to go, but they were not being faxed immediately to physicians. The system had been set up to fax all reports during a nightly run starting at 6 p.m. Making changes to the delivery protocols was not as easy as flipping a switch. To be considered were compliance with the U.S. Health Insurance Portability and Accountability Act, system capability, physician preferences and the effect of interruptions of physicians’ office faxes during business hours. All these had to be addressed to make the change work. With much effort and coordination, the team worked through the issues one by one and now reports are sent out immediately after signature.
After months of implementation, the team was feeling the impact. Physicians were happy. Patients were happy. The team had moved the metric from an average of 64 hours, to an average of 9 hours (Figure 3). This equated to an 85 percent improvement, far surpassing the goal that the team had set.

Control Phase of Project
Sustaining change is often the hardest part of any improvement project. Success requires solid metrics to drive behavior, visibility of progress and strong leadership support. All of these are in place at this Bay Area outpatient imaging center. Three months after the project, the director of the facility said, “We have continued to get great feedback from the physicians. Physicians are now wondering why they do not get the same turnaround from some of our other facilities.” The challenge now for this facility is to transfer what it learned to the organization’s other outpatient sites, and at the same time to continue to listen and act on the feedback from its customers.