
What happens when an emergency department (ED) undergoes major upheaval in the midst of a Six Sigma project? Just such a situation befell a newly trained Black Belt who was working on her first project at Memorial Hermann Southwest Hospital in Houston, Texas, USA.
- One month into the project to reduce cycle times, the ED director, who was the project sponsor, departed.
- Two months into the project, the hospital administration overhauled the ED process flow.
- Three months into the project, a portion of the ED was closed down and a new director was named.
After being compelled to reset her project several times, the Black Belt faced a progress report deadline. Arguably, selection of a project within such a potentially unstable area should never have occurred. But it did and unfortunately, despite the challenges, the project now had to make some progress fast.
Deciding on a Kaizen Effort
To deliver a quick assessment of the current state of the emergency department and create solutions, the Black Belt decided to apply Lean concepts. With consultant assistance, she led a Kaizen event and delivered ED improvements in three areas in only four days.
A Kaizen is a directed effort that applies Lean principles to assess a value stream, identify sources of cost and waste, and reduce those sources, all within a short time frame. The Black Belt and her team began with an assessment of ED processes, including development of a:
Process map: An ordered map of each step that makes up a process.
Spaghetti map: A graphic showing the movements of the patients and caregivers.
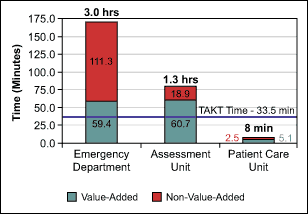
Time value analysis: A chart identifying time spent on value-added and non-value added activities (Figure 1).
Value stream map: A representation of the patient, caregivers, supplies and information flows including time value analysis components (Figure 2).
The spaghetti map illustrated the significant number of moves that caregivers and the case manager applied to treat a single patient. Also of note were the numerous coordinations that occurred. As tangled as the spaghetti map was, the time value analysis was even more telling in that more than two hours of a four-hour patient stay was non-value-added time, that is, time when the patient was not being treated by a caregiver. This time was primarily spent waiting for caregivers or for the results of tests. Most of this waiting occurred during the time in an emergency room.
Seeing What Needed to Be Addressed
The value stream map gave a clear picture of the number of telephonic and manual coordinations needed at each step. Most of these coordinations were rework, following up on testing, coordination for transportation, and placement in an inpatient bed.
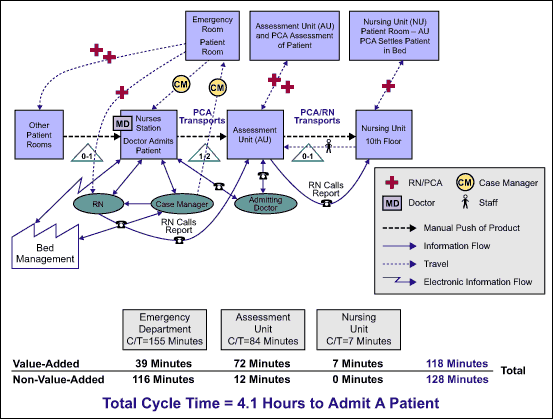
From this assessment, the major opportunity areas for improvement were identified as:
- General layout of rooms in the emergency department not supporting ease of patient care.
- Multiple coordinations and wait associated with arranging transportation.
- Limited emphasis on securing an inpatient bed leading to long wait times.
With the opportunity areas identified and agreed upon, the team was ready to move onto the Kaizen improvement phase. The improvement phase was a planned three- or four-day event where key process owners were brought together under the guidance of a Lean expert, improvement areas were organized and assigned, and teams worked toward implementing solutions.
The key differentiation between a Kaizen and typical improvement approaches is that solutions are actually field tested and evaluated during the Kaizen event. This allows the team and process owners to immediately evaluate the effectiveness of the solutions and adjust as needed. The outcomes of this intensive effort are agreed-upon approaches fully implemented and accepted by the process owners. In the case where a significant investment or extended implementation times are required, the team develops a follow-up plan and transfers ownership to the project sponsor.
Standardizing ED Room Layout
The team first worked on standardizing the examining room layout. This began with a walk-through of an exam room and understanding the equipment and supply needs of the physicians and nurses. Everything else was cleared out, creating open space to allow easy access. Additionally, rooms were stocked with routine-use supplies to reduce trips to the central storage room. A procedure also was established to restock supplies on a daily basis (Table 1).
| Table 1: Standardizing Layouts and Stocking Exam Rooms | |||
|
Operation |
Problem |
Actions Taken |
Results |
| Supply Use | Inefficiencies in collecting non-chargeable, non-regulated supplies | — Remove unused equipment — Standardize layout, labeled, set par levels and reviewed procedure |
— Increased nurse satisfaction — Reduced trips to supply room |
Streamlining Patient Transport
To streamline transportation, the team first released the ED-dedicated transporters to the central pool, but reset the expectation that a transporter would respond to a request within 15 minutes. The second change involved establishing a procedure and training the emergency department staff in the same transportation request system used by other departments. The transporter response rate is being tracked, and transportation by patient care associates and nurses has been reduced to the floors, allowing them to focus on patient care (Table 2).
| Table 2: Establishing a Transportation Procedure | |||
|
Operation |
Problem |
Actions Taken |
Results |
| Emergency Department Transport | Nurses and patient care associates are transporting patients once they are admitted which decreases nurses and patient care associates time in the emergency room | — Pilot solution of using hospital transportation via the PERQs system — Implement using the same protocol throughout the hospital |
— Cycle time decrease of 101 minutes from care complete.until patient departure from the ED — Testing assigned to complete transport in 10.4 minutes |
Focusing on Bed Management
Addressing bed management, the team built a procedure and expectations around the bed assignment process, as well as improving communication between the ED staff and bed management. This primarily involved leveraging the existing ED information system and the visual cues that were available but not understood or acted upon. With education, cheat sheets and clearly communicated expectations, bed management is expediting needed coordination to move care-complete patients to inpatient beds (Table 3).
| Table 3: Leveraging the Existing Emergency Room Information System | |||
|
Operation |
Problem |
Actions Taken |
Results |
| Communciations: ED and Bed Management | — Patients are waiting 143 minutes to depart the ED after care is complete — No standard process or targets — Lack of understanding of symbols on MedHost dashboard |
— Put in place standard operating procedures — Orient staff on key dashboard symbols — Create “cheat-sheet” for symbols and post at every computer |
— 71 percent reduction (shown during pilot) of time from care complete to patient departure from the ED |
Evaluating Improvement Benefits
The final step of a Kaizen is to evaluate the benefits associated with the improvements. This is typically measured in the reduced non value-added time that becomes available for increased value-added activities – in this case, direct patient care.
The improvements and benefits for the ED Kaizen were estimated as:
- Standardizing layouts and stocking exam rooms resulted in elimination of trips to central supply and increased nurse availability by 35 hours per week.
- Establishing a transportation procedure resulted in elimination of transports and increased availability of patient care associates and nurses by 84 hours per week.
- Leveraging the existing ED information system resulted in an accelerated coordination of inpatient beds, or a 71 percent reduction of cycle time, to an average of 42 minutes.
There also has been a routine increase in staff satisfaction as they have made their jobs easier and more fulfilling.
Lean offers a lens to evaluate a process through the eyes of the customer and uncover sources of waste, which leads to patient and staff dissatisfaction. Applying a Kaizen to initially measure, then improve a process offers a method to quickly focus on eliminating waste and accelerating cycle times. And, in this case, the Black Belt was able to deliver the needed improvements on time to the emergency department.