
Contaminated needle sticks are a risk for healthcare workers. These injuries are frightening because the patient whose blood was pricked into the nurse, medical assistant, lab tech or other healthcare worker can be contaminated with Hepatitis B or C, or HIV/AIDS. Once the blood-borne pathogen exposure has occurred, the employee has to undergo tests to rule out these diseases. The employee may have to take antiviral medications, which can cause severe nausea, vomiting, and weakness, until their tests come back and until the patient’s blood is tested. The employee is unable to work during this time. Because of their potentially devastating consequences, these injuries must be prevented.
In 2000, Broward Health’s Environment of Care (EoC) Key Group, the organization’s corporate-level safety committee, challenged the healthcare system to reduce contaminated needle sticks. The organization was to get historical data on these injuries, analyze the causes, and create processes and procedures to prevent them.
Pre-project Work
Workers compensation records, along with the employee health nursing department, were able to supply the exact cost of each needle stick case over the past several years. A preliminary estimate of the cost savings for a project must include lost time, medical care, lab work, medications and transportation. In this case, it seemed possible that $50,000 a year could be saved or avoided by eliminating these injuries.
As part of the pre-project work, the EoC Key Group drafted a preliminary project charter, which included the mandate to review all records relating to the contaminated needle sticks, including the creation of a list of the activity being performed, the device used, the worker job title, and how, when, and why the stick occurred. From this data, the team would create prevention measures involving the key stakeholders in this endeavor and include the manufacturers and suppliers of the devices. In addition, a Safe Needle Device Committee was formed to study new safety devices on the market.
The EoC Key Group expected the project team to create a Gantt chart with a list of tasks, sub-tasks and projected timelines for completion. They also decided to ask the project team to report regularly on the project, showing in-depth knowledge of causes, contributing factors, and methods of prevention and education.
Define
The EoC Key Group, the project sponsor, named a team consisting of safety officers, nursing, workers compensation, infection control and employee health staff. The team also could call upon ad hoc members from the lab, interventional radiology, respiratory therapy, finance and purchasing departments. The team members were familiar with employee accident reporting, workers compensation tracking, OSHA recordkeeping, and the multiple processes and procedures that require the use of needles. They were trained in the concept of measuring defects per million opportunities (DPMO), Six Sigma and the DMAIC roadmap.
The team started the project by creating a process map to illustrate all of the occasions a healthcare worker can be stuck by a sharp or needle. Each step in the processes for drawing blood, administering an injection, starting an IV, removing an IV, obtaining arterial blood gases, and obtaining cultures and specimens was listed. Danger areas were noted, including needle disposal.
Beginning in 2005, all four hospital safety officers added a needle stick metric to the corporate-level dashboard. They measured and reported the number of contaminated needle sticks to the Key Group with a normalizer of 10,000 adjusted patient days (APD), and went back to data from 2000, setting a threshold rate of 3.00 (contaminated needle sticks per 10,000 APD). The threshold not to exceed was set at 3.00 because this was the highest historical level. Since 2001, the hospitals have been below the threshold.
After compiling system-wide data, the team noticed a slight increase (17 percent) in the number of sticks in fiscal year ’04, so they drilled down to determine the root causes and created a Pareto chart of the causes.
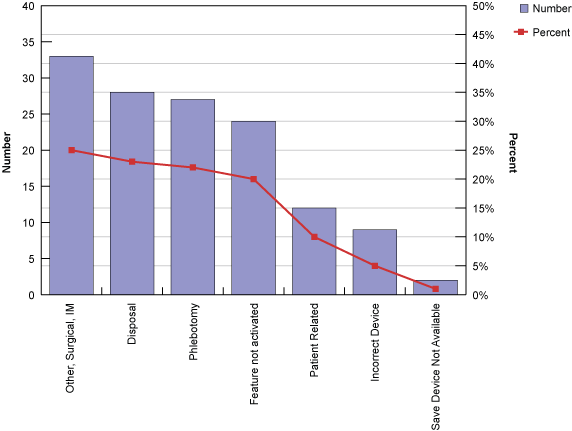
Most sticks were due to unsafe passing of sutures or instruments during surgery and the use of non-safety intramuscular (IM) needles. The next most frequent cause was disposal related, including four sticks from needles being placed in the trash impacting environmental services staff.
Measure
The team was able to define contaminated needle sticks as defects in the system in the provision of care. They found that the opportunities for error were one stick per employee per workday. The team also measured the sticks against 10,000 APD. This metric is used for other quality measures at Broward Health, so proves to be readily identifiable by management.
Based on hospital data, the team found that contaminated needle sticks were 10 to 12 percent of all health system injuries for fiscal years 2005 through Q1 2010. They also found the DPMO and sigma level for the needle sticks (Table 1).
| Fiscal Year | Opportunities for Error | Defects | Contaminated Needle Sticks per Unit | DPMO | Process Sigma |
|---|---|---|---|---|---|
| 2005 | 1,201,000 | 86 | 0.000057 | 57 | 5.36 |
| 2006 | 1,482,500 | 97 | 0.000065 | 65 | 5.32 |
| 2007 | 1,522,500 | 106 | 0.000070 | 70 | 5.31 |
| 2008 | 1,605,250 | 113 | 0.000070 | 70 | 5.31 |
| 2009 | 1,833,500 | 89 | 0.000049 | 49 | 5.40 |
| 2010 YTD | 457,746 | 20 | 0.000044 | 49 | 5.42 |
The team and the Safe Needle Device Committee studied safety device use, provided new safety devices and watched the trends regarding their availability and use. In 2003, nine percent of contaminated needle sticks were due to lack of an acceptable safety device and 10 percent were due to using the safety device incorrectly.
In the years that followed, numerous safe needle devices and needle-less devices were obtained and evaluated over several years as they became available. The team and stakeholders tested and purchased devices consistently after demonstrations by vendors and trials by multiple nursing and lab staffs throughout Broward Health. The team and its counterparts worked with the device vendors and conducted training such that by fiscal year-end 2007 there were no cases of a device not being available and no cases of using a device incorrectly.
The team obtained data on subtasks and cycle time related to contaminated needle sticks from in-depth review of the accident reports and review with the employee health nurses as well as workers compensation. Their records included the tasks involved, the device used, and the narrative given by the injured staff member as to activity and cause. These were measured by number, cost, against manhours worked, adjusted patient days and DPMO.
The team also obtained exact data on the cost of contaminated needle sticks for fiscal year 2006 and the first half of fiscal ’07 system-wide, based on time spent reporting, managing and following up on the exposures; salaries; laboratory testing; and post-exposure prophylaxis. In FY ’06 contaminated needle sticks cost $47,246 for a total of 97 sticks. In the first half of FY ’07 the cost was $39,372 for 47 contaminated needle sticks. That is $86,618 in 6 quarters for 144 contaminated needle sticks. The team determined that the average cost of a single contaminated needle stick was $602.
Analyze
The subtasks involved in contaminated needle sticks were analyzed for the 12-month period of August of 2008 to August of 2009. The team looked at the subtasks involved at the immediate time of the stick (Table 2).
| Subtask | Number | Percent |
|---|---|---|
| Drawing blood | 23 | 26% |
| No explanation | 18 | 21% |
| During disposal | 9 | 10% |
| Using other hand to close safety device | 8 | 9% |
| In the trash, impacing environmental services staff | 6 | 7% |
| During surgery | 6 | 7% |
| After giving insulin | 6 | 7% |
| After giving an injection | 6 | 7% |
| Removing or adding to an IV | 5 | 6% |
| Total | 87 |
Twenty six percent of sticks took place during or just after drawing blood and 10 percent during disposal. However, 21 percent of the cases had no description of subtask involved in the employee accident report. After this the team worked with the managers, employee health nurses and workers comp to get all the necessary data.
The team informed nursing, laboratory and respiratory therapy managers that drawing blood was the most-frequent subtask involved in sticks. The team also spoke with purchasing and learned that their Value Analysis Committee (VAC) was bringing in a new vacutainer needle for drawing blood. They hoped this tool would greatly reduce sticks.
The project team also conducted benchmarking and researched related literature. In 2000, Linda Rosenstock, the director of the National Institute for Occupational Safety and Health wrote, “needle stick injuries are contributing to the overall burden of healthcare worker injuries. Although we do not know exactly how many work-related needle sticks occur each year across the country, estimates indicate that 600,000 to 800,000 such injuries occur annually, about half of which go unreported.” (Rosenstock)
This article also helped the team to benchmark the healthcare job titles involved in needle sticks. Rosenstock said, “most reported needlestick injuries involve nursing staff; but laboratory staff, physicians, housekeepers and other healthcare workers are also injured. Healthcare workers outside the hospital setting are also at risk. Others at clinics, private medical and dental offices, nursing homes, correctional facilities, and in the community, such as emergency medical response workers, are also at risk of exposure to contaminated blood.”
To benchmark the tasks involved, data from two surveillance programs, the CDC National Surveillance System for Healthcare Personnel and EPINet, a project developed by Dr. Janine Jagger at the University of Virginia, provided descriptive epidemiological evidence of how such injuries occur, including under what circumstances, with what devices and during what types of procedures. “The picture that emerges reflects a continuum of risk opportunities throughout the life-cycle of sharp device use involving interactions among patients, workers, devices and the environment.”
Through further benchmarking research, the team found a study funded by the CDC that examined needle stick injuries in an acute-care community hospital in greater Washington, D.C., from 1990 to 1998. The study found that implementation of a multi-faceted intervention program led to a significant and sustained decrease in the overall rate of sharps injuries. Annual sharps injury incidence rates decreased from 82 sharps injuries/1,000 full-time employees (FTEs) to 24 sharps injuries/1,000 FTEs, representing a 70 percent decline in incidence rate overall.
The team also investigated benchmarking data from the Canadian Center for Occupational Health and Safety. Their preliminary findings were that the Broward Health system sharps incident rate and contaminated needle stick rate was anywhere from equal to or 82 percent lower than those benchmarked, depending upon metric and denominator.
Improve
The recommendations made to stakeholders involved trialing and implementing safety devices, training of staff in those devices, conducting repeated training, and ensuring awareness of the user errors and techniques involved that lead to the sticks. Even after safety devices are implemented, user error is common.
Training and awareness involved new-hire orientation and ad hoc information dissemination on the causes of contaminated needle sticks. Slides, shown below, were sent system-wide and are used in nursing new-hire orientation.
|
Prevention of Needle Stick Injuries Did you know, all contaminated needle sticks are due to technique/user error?
|
|
Prevention of Needle Stick Injuries Did you know, all contaminated needle sticks are due to technique/user error?
|
|
Safe Sharps Disposal – Prevent Contaminated Sticks While wearing gloves:
|
Piloting of safe needle devices and needle-less devices took place over nine years as devices were introduced by vendors. Training in these devices was conducted regularly by the clinical education department and the vendor representatives. The awareness slides were piloted and fully institutionalized into in-service education sessions. The results were monitored in monthly meetings held by the Safe Needle Device committee and their findings were reported to the EoC Key Group on a quarterly basis.
We believe that we have successfully met the challenge of reducing contaminated needle sticks, while attending to patient comfort and safety, and reducing costs to Broward Health.
Control
Controlling exposure to contaminated needle sticks is assured only by institutionalizing the policies and procedures established by the performance improvement process.
The team and management are committed to making sure safety devices are in place and utilized. The team will continue working with the purchasing department VAC regarding new devices as they become available. Continuing the training and awareness in classroom and online programs also is critical to quality.
The safety officers, workers compensation and employee health nurses will constantly observe, track and report all sticks and their cause and source. The rates are reported quarterly at each of the five regional EoC Committees and to the Key Group.
Contaminated needle sticks are treated as defects in the healthcare delivery system and the rates are presented in occurrences per 10,000 APDs at the hospitals. The team also tracks the cost per needle stick. The number of sticks went down 21 percent FY ’09 over FY ’08, but the costs went up 29 percent over FY ’08 due to treatments for HIV and lost time. However, overall, the team could show that their efforts have avoided $135,942.00 in cumulative costs to Broward Health year over year from the baseline of $78,798.00 in needle-stick related costs in 2000.
The contaminated needle stick injury rates are on the corporate dashboard that goes up to the Board of Directors and the Quality Assurance and Oversight Committee. The CFO has asked for quarterly cost savings metrics in the Environment of Care and the cost of contaminated needle sticks is one of those metrics to track that rates remain in control.
References
- Canadian Centre for Occupational Health & Safety, January 25, 2005
- CDC National Surveillance System for Healthcare Personnel
- Infection Control and Hospital Epidemiology, July 2007
- Jagger, Janine, PhD EPINet, University of Virginia
- Rosenstock, Linda. STATEMENT FOR THE RECORD ON NEEDLESTICK INJURIES National Institute for Occupational Safety and Health Centers for Disease Control and Prevention, U.S. Department of Health and Human Services. June 2000