
The quality and variability of care delivered by hospitals is highly profiled in the media today. Pick up a newspaper, turn on the television or open a healthcare trade journal and chances are there will be an article detailing the real or possible occurrence of medical errors, allegations of a hospital’s failure to comply with federal or state regulations, or some other issue questioning the quality of medical care.
A significant portion of the public has not simply lost confidence in hospitals, but thinks they actually can be dangerous places. In its 1999 report, “To Err Is Human,” The Institute of Medicine validated such public perceptions by noting that as many as 98,000 Americans die annually as a result of medical errors.
It has been almost 20 years since hospitals began adopting formal quality models such as Total Quality Management (TQM), Continuous Quality Improvement (CQI) and Plan-Do-Check-Act (PDCA). During this time, hospital quality improvement programs have expanded their use of measurement tools and process design techniques. Despite such efforts, many successful programs are now recognizing that a higher level of rigor and sophistication is required. Thus many hospitals are embarking on a cultural change grounded in Six Sigma concepts and principles to catapult themselves into a new, higher dimension of quality.
While Six Sigma and traditional quality models are complementary and build on the traditional set of tools, there are some key differences:
| Traditional Quality Programs | Six Sigma |
| Initiatives Identified Internally | Initiatives Determined by Customer CTQs (Critical to Quality Elements) |
| Sidebar Activity, Often Separated from Business Strategy |
Integral Part of Organization’s Culture and Business Strategy |
| Focus Is on Moving the Average | Focus Is on Eliminating Variation in Customer CTQs |
| Departmental Activity | Emphasizes Cross-Functional Process Management |

Six Sigma offers two similar-but-distinct-models to use, depending upon the nature of the project. Initiatives focused on improving existing processes follow a DMAIC (Define, Measure, Analyze, Improve and Control) model; initiatives focused on the development of a new process, such as those related to a new program or new service, follow the DMADV (Define, Measure, Analyze, Design and Verify) model.
A case study illustrates how a healthcare Six Sigma project team applied the DMAIC approach to improving the care of open-heart surgery patients by reducing their post-operative length of stay. The case study follows the process step by step:
The Define Phase
There are four key steps in the Define phase of the DMAIC process:
- Identify the process or product for improvement.
- Identify key customers and those elements viewed as critical to quality.
- Develop a team charter with problem/goal statement, project scope, business case, team roles and milestones.
- Develop a high-level process map for the most significant four or five steps of the process.
In this case, the team’s objective was to increase the quality of patient care while reducing the average length of stay and costs for open-heart surgery patients. This had been the objective behind several initiatives in the past at this particular hospital, many of which – such as the implementation of critical pathways – had been successful.
However, a comparison of the hospital’s length-of-stay data to “best practice” hospitals revealed an opportunity for further improvement. The comparison indicated that 53 percent of the hospital’s patients were discharged on or after the seventh post-op day compared to 18 percent for benchmark hospitals. (Figure 2) In addition to improving the quality of care, the potential economic opportunity to the hospital was estimated to be $400,000 annually. This financial value was calculated by multiplying the cost per day by the projected number of days to be saved through this performance improvement initiative. The economic impact to the hospital combined with increased competition from neighboring cardiovascular centers and declining program reimbursement, convinced the hospital administration to charter a special project team to work on this initiative.

At the first team meeting, the project leader reviewed the charter with the team members to ensure clarity of purpose, goals and the parameters or scope of work involved. A process flow map also was completed. (Figure 3) The development of the process flow map was a valuable exercise – especially for team members who were getting their first view of the entire process and the role they played.
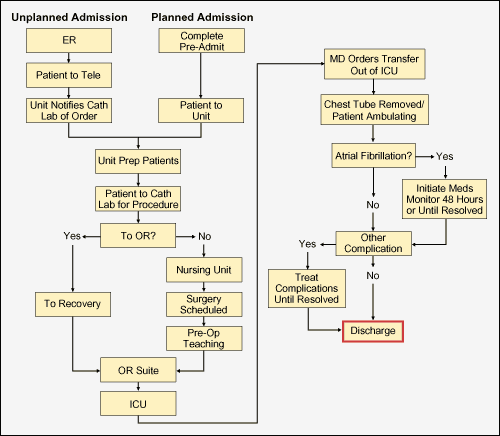
The Measure Phase
All processes can be viewed as a series of inputs or factors (x’s) contributing to the output (Y). In other words, every process can be expressed in terms of the mathematical equation Y=f(x), where Y is a function of x. In this case, example Y was post-op length of stay for open-heart patients measured in days, and the x’s were the various factors contributing to length of stay.
The team’s next step was to identify all the factors (x’s) potentially impacting the post-op length of stay (Y) by completing a cause-effect fishbone diagram. (Figure 3)
The fishbone diagram was a useful technique in helping team members articulate all the possible contributors to post-op length of stay versus the few that typically come to mind. Completion of a fishbone diagram also is essential in identifying all the potential contributors to process variations – a fundamental principle of the Six Sigma approach. For example, in this case, some of the x’s included atrial fibrillation, time of extubation and attending cardiologist.

The Analyze Phase
Once all potential contributors of variation had been identified, the team turned its attention to identifying those that most significantly contributed to a longer length of stay. Identification of the critical factors (x’s) having the most statistically significant impact on process variation is the key component of the Analyze phase of the DMAIC process. The team discovered that atrial fibrillation and lack of ambulation were driving much of the variation in length of stay.
It was from this analysis of key factors that the hospital was able to create new operating procedures to reduce variation in the management of atrial fibrillation and the less obvious area of patient ambulation. Through the rigor of this statistical analysis, data was used to communicate to key stakeholders (physicians, hospital staff, patients) the need for a consistent process where no formal process had existed. While not very surprising, patients with atrial fibrillation stayed more than two days longer than those without – 6.9 days with atrial fibrillation, 4.6 days without.The more interesting finding was that those who did not ambulate also had a two-day difference in length of stay – 6.8 days with no consistent ambulation, 4.8 days with consistent ambulation.
The Improve Phase
Armed with this information, the team concentrated its improvement efforts around those areas known to be the most significant contributors to variance. A standard operating procedure related to ambulation of patients was developed and implemented, with accountability clearly identified. A protocol for treating atrial fibrillation was developed in conjunction with the medical staff and disseminated to all stakeholders. It was this communication to stakeholders that really began to drive change within the organization. A previously unknown factor was found to be significant, and this translated into a new process and improved performance.
The Control Phase
The Control phase is perhaps the most important part of the DMAIC process. It also is the step most frequently overlooked. In this case, data collected during the Define and Measure phases indicated that the probability of a post-procedure length of stay of greater than 6 days was 0.18. After improvements were put into place, the probability of a length of stay of greater than 6 days was 0.13. The percentage of patients with post-op stay greater than 6 days fell from 53 to 22 percent.
With the project now in the Control phase, the team will continue to monitor a dashboard of performance indicators on post-op length of stay, adherence to the atrial fibrillation protocol and ambulation to make sure that procedures are followed and improvements are sustained. The team will report regularly to key stakeholders to maintain effective communication and address any performance issues as necessary. Because the key factors causing variation have been identified, ongoing performance monitoring can focus on those critical areas, thereby improving overall efficiency.
Summary
This case study is just one of many examples that illustrate the impact of Six Sigma within the healthcare environment. It is a methodology which helps hospitals continually evaluate how they are performing, improve the effectiveness of quality initiatives, and renew employee spirit by creating a culture based on the core value of health care providers – delivering the highest quality of care, compassionately.
And importantly, these improvements are what communities want and expect from their local hospitals…the things which reinforce public confidence in all hospitals.