
When confronted by concerns of some physicians about frequent lengthy delays that they experienced admitting patients, Memorial Hermann Southwest Hospital in Houston, Texas, assembled a cross-functional Six Sigma team to identify and address any underlying issues that might be causing the delays. The business case for pursuing the project was clear. Improving bed management and availability aligned with the organization’s goal to become a destination hospital where employees want to work, patients want to receive care and physicians want to practice.
Scoping the Project
As the team began setting parameters for the project, it had to take into account the physician complaints that patients had to wait in the physician’s office or assessment unit for a bed to become available. The team had to then determine whether it should concentrate on admission or discharge, or perhaps something occurring in between. The team decided to focus on the ability to discharge patients in a timely manner, which it turned out was one of the key drivers for admission delays.
The project was scoped from the time the physician wrote the discharge order to the time the bed was clean and available for the next patient. Measurement system analysis indicated zero errors, since a time stamp automated the final step. The first step was simply observing the time physicians wrote down the order, and that was successfully completed.
Initial data collection for the project included gathering internal information on discharging patients and reviewing similar Six Sigma projects from other healthcare facilities. The team discovered the hospital had significant opportunities for improvement, and was surprised at how long it took to actually discharge a patient.
Define and Measure Phases
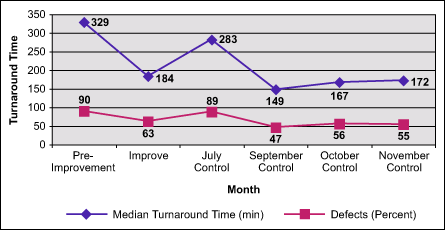
During the Define phase, data revealed it was taking roughly 7.5 hours from the time a discharge order was written to the time a bed was available for the next patient. The data was non-normal, and the median was 329 minutes in the Measure phase. The goal the team established was based on benchmarking the time required for different processes, and the upper specification limit was set at 150 minutes.
The process was broken into four phases, each targeting separate sub-Y’s:
- Order written to noted in chart
- Noted in chart to patient leaving
- Patient leaving to entered in computer
- Entered in computer to bed clean
Each step was closely examined and assigned upper specification limits. Initial capability analysis revealed 90 percent defects, or 909,000 DPMO (defects per million opportunities). The sigma level was essentially zero, but the team gave themselves credit of.2 sigma to start. The performance objective was to reduce defects by 80 percent, reaching 2.41 sigma or 18 percent defects.
This was admittedly a tall order, but the team knew the current state was unacceptable. Critical factors included the gap in time between the patient leaving and having the information entered in the computer, and the actual bed cleaning time. The team initially thought housekeeping would be one of the most efficient aspects of the project, but it turned out to have the most variation. It took an average of 245 minutes to clean the bed, and with an upper specification limit of 85 minutes this became a major focal point.
There were many stakeholders to consider as the team moved through each phase of the project, including nursing staff, patient care attendants and technicians. To understand each group’s concerns, the project team completed a stakeholder analysis, collected voice of the customer data and involved key people on a regular basis, such as physicians, intensive care unit staff, telemetry staff and administration.
Floors 6 and 10 of the hospital were identified as having the greatest opportunity for improvement. A cause-and-effect matrix and detailed process map were developed and reviewed for accuracy with staff.
Analyzing and Addressing Opportunity
During the Analyze phase, a Work-Out session was conducted to address use of the interactive voice response (IVR) system to discharge patients. With IVR, the caregiver calls from the patient’s room as they are about to leave, immediately notifying housekeeping to begin the cleaning process. Prior to the IVR system, the floor nursing staff would have to communicate to the central desk that a patient was leaving. The central desk would then enter the discharge in the computer.
Delays meant it could take up to an hour and a half for notification to occur. A successful pilot of the IVR system on the two target floors led to subsequent implementation across the hospital.
Another opportunity involved a post-discharge lobby for patients who had received their discharge order. When the team analyzed utilization, it found only 20 percent compliance, so increasing usage of this lobby became one of the targeted improvements. By the time the project was completed, they were able to achieve 80 percent compliance.
Within the bed cleaning process, six opportunities for improvement were identified. Initial data collection uncovered an average of 150 “stat cleans” per week. This was key, since beds without stat orders were not being cleaned. An approval process was put in place to qualify such orders, and they went from 150 stats a week down to eight. Utilizing the zone supervisor function in the ABC bed tracking system also was helpful. If a room were not put in progress within 30 minutes, the two managers on site would be paged and could respond quickly.
Unfortunately, vacancies are a consistent issue in housekeeping and obviously a factor in having the rooms cleaned in a timely manner – either due to staff shortage or variability in carrying out procedures. Four vacancies were filled during the course of the project, though others have come up since then. Attention to this area can make a significant difference.
The team also explored staffing patterns and shifting of resources. Because of the pilot on the two target floors, the team knew peak discharges were occurring within the 2-to-4 p.m. period. Staffing, however, was concentrated in the period between 6 a.m. and 2:30 p.m. With changeover during peak times there sometimes were not enough people on the floor. The team decided to shift resources and have two people come in from 7 a.m. to 3:30 p.m., and also had a discharge planner available from 3 to 11 p.m. and 1:30 to 9 p.m.
It usually took 30 minutes from the time housekeepers arrived in a room to the time they left, so this was not the bottleneck in the process. There is a standard way to clean the room, and they all follow that routine. Delays occurred in getting to the room to begin cleaning, and then afterward making sure the notification was done promptly so a new patient could be admitted.
Along with changing processes, the team had to educate and set new expectations. Housekeeping staff had been trained that turning rooms within two hours was an acceptable goal. With the new target of no more than 85 minutes, staff would need to understand why the changes were important to the hospital and patients.
Improving and Controlling Results
The project to improve bed availability which began in 2004 at Memorial Hermann Southwest Hospital produced significant results. Patients do not have to wait as long to get into a room once the physician has given the order for admission. Defects in the overall process have been reduced from 90 percent to 55 percent, and median turnover time decreased from 329 minutes to 179 minutes.
Productivity has increased in housekeeping, and feedback collected during the Improve phase helped to verify that satisfaction for physicians and patients has risen as a result of changes that have been implemented.
One physician remarked at the outset of this project that bed availability was a problem most of the time and that it could take hours to get a patient into the hospital. A follow-up comment from this same physician indicated the situation had greatly improved and he was not encountering difficulties admitting patients.
In July 2005, the team’s first Control measure indicated that the process had reverted back toward its previous state, which was unacceptable. The Black Belt immediately called a meeting with the Green Belts, project sponsor and executive Champion to address the issue. It was determined that variation had slipped back into the process due to a significant change in nursing management across the hospital.
New people were now in charge and unaware of the improvements put in place. An action plan was developed to focus on re-education and consistent process monitoring, so that improvements could be sustained in the future. Through additional monitoring, the team was able to verify that the plan worked, and the process continued to improve beyond initial measurements.
Memorial Hermann Healthcare System maintains an enhanced discharge team, with representatives from each hospital. Once the bed availability project entered the Control phase, it was transitioned to this team for monitoring and analyzing other pieces of the process. Automation with IVR is being institutionalized across the entire health system, with discharge care sets that alert the nurse regarding steps that should be taken in order to properly discharge the patient from the hospital.
The admitting project was part of a larger, system-wide improvement initiative that began in 2004. The program has greatly improved collaboration, communication and best practice sharing throughout the organization. Beyond individual project results, people at all levels feel more empowered and equipped to solve problems. They have embraced a common language and toolset for leading change and creating the optimal environment in which to deliver and receive care.