Cardiovascular disease is the leading cause of death in the United States, and more than 900,000 people annually are diagnosed with acute myocardial infarction (AMI). The Joint Commission on Accreditation of Healthcare Organizations (JCAHO) and the Centers for Medicare and Medicaid (CMS) have identified AMI as one of the early priority focus areas for hospital core measure development.
The timing of reperfusion is critical to the effective management of AMI patients. The earlier therapy is initiated, the better the outcome. Patients presenting with AMI and ST-segment elevation or left bundle branch block are at a relatively high risk of death. This risk may be reduced by percutaneous coronary intervention (PCI), but only if it is performed in a timely manner. The timeliness of reperfusion is one of the AMI treatment issues addressed in “Healthy People 2010,” a government report of national health objectives, which identifies the most significant preventable threats to health.
At Deaconess Health System in Evansville, Indiana, USA, a Six Sigma team began a door-to-inflation project focused on the patient throughput process from the time the AMI patient arrived at the emergency department until inflation of the artery occurred in the cardiovascular lab.
In the Define phase (of a DMAIC [Define, Measure, Analyze, Improve, Control] project), Green Belts walked through the process and obtained the voice of the physicians and staff from the emergency department and cardiovascular lab. While analyzing the data, the team identified a significant opportunity to reduce wait time when the emergency department and cardiovascular lab share responsibility for tasks between the two areas. The team used Work-Out to allow emergency department staff and cardiovascular lab staff to identify a standardized, consistent process that reduced wait times and improved patient throughput.
An overview of the project demonstrates how the Six Sigma DMAIC methodology provided Deaconess with the framework and tools to decrease door-to-inflation times and meet the CMS target for this core measure.
Defining the Problem
Door-to-inflation throughput was selected as a project by Deaconess Hospital for several reasons, including the opportunity to improve patient outcomes, growth in PCI volume, and preparation for future CMS pay-for-performance efforts based on the indicator. The organization wanted to ensure that the emergency department and cardiovascular lab could consistently provide timely, quality patient care and meet the CMS target for emergency PCI patients.
Management from both areas believed that opportunities to increase efficiencies and throughput existed. The goal was to improve PCI patient throughput time, which would result in improved outcomes.
A team charter was written and approved by administration. Four Green Belts were selected to work on the project and train with the system’s Six Sigma consultants.
The charter included:
Project scope – Includes all processes beginning with the AMI patient arriving in the emergency department and ending with inflation in the cardiovascular lab.
Problem statement – The average throughput time of the AMI patient with diagnostic EKG does not consistently meet the CMS target.
Goal – Reduce the average time for an AMI patient with a diagnostic EKG, from arrival in the emergency department to balloon inflation in the cardiovascular lab.
Team members – The team consisted of the four Green Belts, managers and staff from the emergency department and cardiovacular lab, and call center staff. Serving as the project Champions were the vice president of nursing, the director of the emergency department and the director of the cardiovascular lab. An emergency department physician and cardiologist served as physician Champions; their active participation and support were key elements in the success of the project.
The process map pointed the team to three areas of focus – interventional cardiologist on first call for the AMI-8 patient, standardization of the process between the emergency department and cardiovascular lab, and a flow sheet with feedback to the staff and physicians.
Measurement and Analysis of the Data
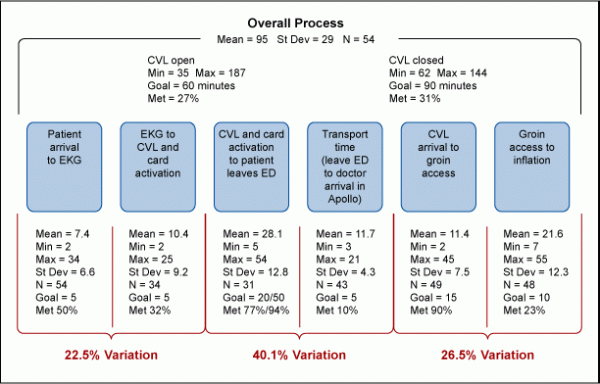
The team created a value stream map (Figure 1) of the six sub-processes:
- Patient arrival to EKG
- EKG to activation of the cardiovascular lab team and cardiologist
- Cardiovascular lab team and cardiologist activation to patient leaves emergency department
- Transport time from when patient leaves emergency department to arrival in the cardiovascular lab
- Cardiovascular lab arrival to groin access
- Groin access to inflation
While analyzing the data by subprocess, the Green Belts found that 40 percent of the variation in the process was occurring when the two departments shared responsibilities. Data and voice of the staff revealed that opportunity areas were:
- Cardiovascular lab team and cardiologist not being notified at the same time.
- A non-interventional cardiologist being called first, then calling an interventional cardiologist.
- Lack of a standardized process for handling the AMI patient with a diagnostic EKG.
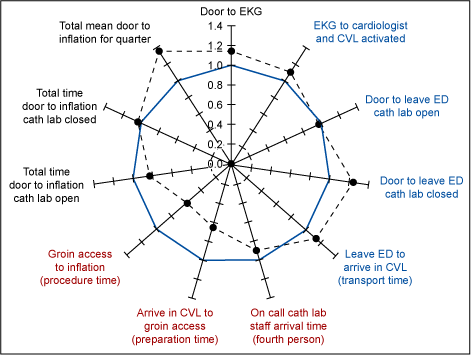
The team benchmarked both internal and external sources for best practice. One internal benchmark was Deaconess trauma services. Ideas such as simultaneous notification of the trauma surgery and trauma team, emergency department and surgery staff sharing the process, and immediate feedback to the trauma team were leveraged for the door-to-inflation process. The JCAHO core measure benchmark for AMI-8 patients is 120 minutes from door to inflation.
The team Champion, Sponsors and Green Belts redefined the project goals based on their benchmark findings, data and voice of the staff. The goals were:
- 50 percent of patients will obtain reperfusion or first inflation within 60 minutes of arrival.
- 75 percent of patients will obtain reperfusion or first inflation within 90 minutes of arrival.
- 100 percent of patients will receive reperfusion within 120 minutes of arrival.
Process Improvements
The Green Belt team made a recommendation and gained approval from their Champion and Sponsors to immediately eliminate non-interventional cardiologists from the emergency department first call list for AMI patients. In order to develop a standardized process for handling the AMI patient with a diagnostic EKG, the team conducted a Work-out with frontline staff. The following improvements resulted:
- An AMI-8 team was formed consisting of the emergency department physician, emergency department charge nurse, interventional cardiologist, cardiovascular lab charge nurse, assistant director of nursing and patient registration representative.
- The cardiovascular lab team and cardiologist are paged simultaneously.
- A standardized process was developed for all AMI-8 patients.
- “We can do it!” immediate feedback form was developed to share with emergency department and cardiovascular lab staff on each AMI patient.
- Monthly feedback is provided to staff and physicians, including graphs showing goals versus actual performance.
Staff was trained on the new standardized process and documentation. The new process was implemented in July 2005. To sustain the improvements, the team developed a control plan that included control charts for total door-to-inflation time and each critical sub-process so the process owners could monitor progress.
These control charts are reported monthly to the director of cardiovascular services and the emergency department, and quarterly to the Health System Quality Council in order to hold the process owners accountable for ongoing results.
Achieving and Maintaining Results
Results after three months showed a significant improvement in door-to-inflation times:
- Reperfusion within 60 minutes improved from 13 percent to 40 percent.
- Reperfusion within 90 minutes improved from 51 percent to 69 percent.
- Reperfusion within 120 minutes improved from 85 percent to 96 percent.
Additional benefits gained from the project are increased physician and staff satisfaction. The AMI-8 team now has a standardized process, with the team working together to expedite the patient from door to inflation in a timely manner. The overall average door-to-inflation time has been reduced from 95 minutes in 2004, to 77 minutes as of September 2005, as a direct result of this Six Sigma project.