
As with most hospitals, labor is the largest budget expense at the Providence Alaska Medical Center (PAMC) in Anchorage. But benchmarking indicated that staff utilization at PAMC, a part of the Providence Health System, was above the 75th percentile of the national average. To remedy this, in October 2003, a multidisciplinary team (nursing, leadership, finance and physicians) began a Six Sigma project to create a more effective process for scheduling staff.
During the Define phase of the DMAIC (Define, Measure, Analyze, Improve, Control) project, the team found that the hospital’s staffing dollars – which includes salaries, benefits and contract labor – were substantially over budget. Roughly 75 percent of the variance could be linked to nursing salaries and the use of registered nurses from outside staffing resources. Within the nursing area, the team found that the adult critical care unit (ACC) was 22 percent over budget for staffing.
The primary goals or targets for this project as set by the team included:
- Right person, right place, right time to meet quality standards
- Meet budget
- Schedule/forecast staffing needs
One of the key aspects of the Define phase involved learning to scope properly from the broader focus area of staffing effectiveness to real-time schedule management in the ACC. The team accomplished this with initial data collection and hospital financials. As the team moved into the Measure phase, it identified the critical X‘s, and developed a plan to measure and collect the data.
About Providence Health System
Providence Health System provides healthcare services across a four-state area – Alaska, Washington, Oregon and California.
More than 33,900 employees work within these four regions, which are further divided into service areas.
With a total of 3,712 acute care beds, and 1,741 long-term care beds, the system includes 18 acute care hospitals, 12 freestanding long-term care facilities, and 20 low income and assisted living facilities.
The Providence Health System in Alaska was founded in 1902, and has 389 acute care beds and 333 long-term care beds.
Gaining Commitment
Along with the statistical process control that Six Sigma provides, the team knew it would need to address the people side in order to gain acceptance for proposed solutions. To ensure consistent communication and to generate buy-in from the department manager, staff and clinicians, the team used several change management techniques.
The change tools helped to overcome initial resistance – especially from some physicians, who thought they knew the source of the problems, and were anxious to simply implement a solution. The team was able to overcome this potential barrier by applying change management strategies that focus on building acceptance and mobilizing commitment.
To make changes in a 24/7-environment, the change facilitators had to be creative in their approach to brainstorming so that everyone would have an opportunity to provide input. Change acceleration process (CAP) sessions were conducted at different times over many days, and the team placed data and material in the break room to allow greater access to information. Work-out also was useful in formulating solutions based on the Six Sigma data analysis.
Introducing a New Data Collection Process
Before the project, data collection for staff scheduling had been an irregular, non-standardized process. With insufficient or inaccurate data to guide them, charge nurses often made decisions based more on perception than on reality. While there were definitions for the data elements to be documented, they were not printed and readily available, leading to various interpretations and usage of the information.
The team began to develop a new data collection process that would meet its needs and improve the reliability of the scheduling system. The team met with stakeholders and charge nurses, and used brainstorming techniques to understand factors that might affect the charge nurse’s ability to staff the ACC at appropriate RN levels. They then organized the ideas on a cause-and-effect diagram and used multi-voting to determine the key issues according to everyone’s perception.
The next step was to review these issues and determine how to measure them. Data collection was separated into three categories:
- Information that could be obtained from existing hospital systems.
- Information the charge nurses could collect (with minimal interruption to patient care duties).
- Information the Six Sigma team members would collect.
The team created concise data collection forms and standard operating procedures (SOP) for each group, and provided training for data collectors on the new process. One person would check with the charge nurses each shift to answer any questions and review the data collection sheets to see if something looked different. After two weeks, the team members compiled the data from all sources into one master data spreadsheet workbook.
Using a Spreadsheet Workbook
To provide a clear method for tracking the thought and work processes, the workbook included tabs for: master data sheet, SOP, working data sheet, raw data sheets and finally a Minitab data sheet. The SOP tab was helpful as the sheet continued to grow and develop, providing answers to what was happening and why.
The team developed extremely detailed data collection standard operating procedures. One of the things complicating this effort was the fact that the team had to collect many of the data elements over different time frames. For instance, some data points, such as predicting admissions, were collected once per shift (12 hours); some, such as admits, discharges and transfers, were collected over four-hour intervals, while other data elements were collected twice a day to coincide with two 12-hour shifts.
The Analyze phase helped the team to compare its initial theories against rigorous analysis of the problem, using statistical software and process analysis tools. The team looked at the skill mix for the job of patient care tech, health unit clerk and monitor tech. Members also examined the geography of the unit and the distances staff had to travel.
The process analysis revealed that SOPs were needed for flexing staff, predicting patient census and management approval for non-direct patient care time.
Finding Solutions
During the Improve phase, a new staffing grid was implemented. This was based on the number of patients in the unit, also taking into account the number of potential 1:1 nurse-to-patient ratios at each level of staffing.
The final column of the staffing grid had the “hours per patient day = staff-paid hours per number of patient days” calculated so the charge nurse could visually see when they would be over budget and make changes if appropriate.
Two Work-out sessions were conducted during the Improve phase. One involved the nursing management team and focused on creating categories for SOPs and establishing boundaries. A second Work-out with the ACC nursing staff concentrated on completing the details of the SOP and planning process changes.
Far-Reaching Results
As the project entered the Control phase in July 2004, the team sought to establish a simple monitoring process to make follow-through easier. Tools were eventually built to accomplish this function.
Once the team goals were achieved, the charge nurses became more aware of staffing-to-patient volume changes and tracking the ratios every four hours. The medical center is continuing to provide education for nurse supervisors and charge nurses regarding the cost of staff hours worked to patient days.
Both the data collection integrity and focus on the adoption of the process by stakeholders have been instrumental in achieving strong results. The data also was helpful in validating the success of changes in the unit that occurred outside the scope of this project – information that might never have been captured without this effort.
Financial Benefit Calculation
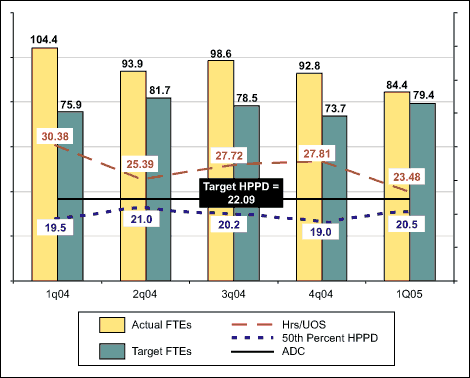
Hours per patient day (HPPD):
From 30.38 in Q1 2004 to 23.48 in Q1 2005.
Average daily census (ADC):
Up an average of 20 points per day.
Average pay rate: $29 per hour.
Calculations:
6.9 HPPD x ADC 20 = 138 HPPD
138 HPPD x 365 days = 50,370 hours/year.
50,370 hours per year x average pay $29 = annual savings of $1,460,730.
Using the new staffing grid, the team had projected an annual financial benefit of $850,000. The actual number was $1,460,730.
| Results of Project Goals | |
| Goal | Result |
| Right person, right place, right time to meet patient quality standards | Designed staffing grid to account for different patient census and acuity levels |
| Meet budget | Saved $1.4 million |
| Schedule/forecast staffing needs | Staffing to grid allows for better decisions |
|
|||||
Conclusion: Keys to Success
Developing an effective strategy for scheduling hospital staff can present unique challenges. During the course of this project, the Six Sigma team discovered some important keys to success:
- Spend sufficient time scoping the project on the front end.
- Begin planning early, including communication strategies to keep all staff informed about the status of the project.
- Apply change management techniques to overcome resistance.
- Consider what will be needed from the data collection and why, to make sure the information gathered will really answer your questions.
- Create written SOPs while processing data to understand the rationale behind each step.
- Make it easier to manage and track information by keeping the data within one spreadsheet workbook, with separate tabs as needed. (Hint: Enter and manipulate the data in a spreadsheet and then migrate final data into statistical software for output.)
The project has had far-reaching results across Providence Alaska Medical Center and has since been translated to many other nursing units. Collectively, the projects have supported the hospital’s objectives of reducing staffing costs and creating culture change…the right person, at the right place, at the right time to meet quality patient-care standards.