
The following is Part One of a three-part article. Click here to read Part Two. Click here to read Part Three.
A chain of medical diagnostic clinics was developed from the ground up. After two years of hectic expansion marked by acquisitions and setting up greenfield clinics across a number of cities, it became clear that due to the different inherited processes across those acquisitions, the chain needed to focus more on improving and standardizing the quality of service offered, and improving its customer satisfaction rankings.
Getting Started
A two-day “quality mindset” program was conducted for the chain’s 20-member senior management group. This program introduced the leaders to the concept of customer delight and its key ingredients – product quality, service, delivery and cost. The program also explained how to improve those ingredients through the application of total quality management (TQM), by incorporating just-in-time (JIT) manufacturing principles, total quality control (TQC) and employee involvement. Most importantly, through interactive exercises, this program helped to open the group to change.
Two specific areas for improvement were selected by management – turnaround time of patients and customer service. These areas of improvement were addressed by 1) working for reduced patient turnaround time at Center A (the chain’s busiest center), 2) improving customer satisfaction at Center B (the chain’s second biggest center) and 3) improving internal laboratory processes at Center A. This case study is organized in three parts to correspond to the three areas of improvement.
To approach the issue of patient turnaround time, the company chose to follow the seven steps of problem solving.
- Define the problem and measure it
- Research root causes (using the 5 Whys)
- Discuss and agree upon countermeasures
- Test countermeasures
- Check results
- Standardize results
- Compile quality improvement story
In addition to these seven steps, the chain also incorporated JIT principles by cutting non-value added stages and activities in the process, reducing work through automation, improving workflow, etc.
A cross-functional team was chosen to work on these improvements and the project began.
Step 1: Define the problem and measure it
The problem was defined as the difference between the desired level of patient wait time and the actual time patients had to wait to finish their diagnostic tests.
The company wanted to reduce the non-value added patient time, which largely consisted of patient waiting time – where waiting time excluded all time that was an essential part of the medical procedure (e.g., two hours of waiting after a meal for a post-meal blood test to determine sugar levels for diabetics).
Measuring the turnaround time of each patient was impractical, however, because it would require a staff member to follow patients one at a time. Instead, a patient’s path and waiting times were determined by their specific test requirements.
The most useful metric the company could analyze was, therefore, the number of patients waiting – which in Lean parlance would be considered work in process (WIP) – at any time. A format was developed to collect this data hourly for one week in the 16 hours the clinic operated each day. From this data the current status was measured as follows.
Number of patients waiting at any given time (WIP):
- Average = 36
- Standard deviation (σ) = 11
- A + 3σ = 69 (refers to the instances of maximum queue length and thus relates to the maximum waiting time and most significant customer dissatisfaction)
It was decided to target a WIP reduction of at least 50 percent.
An Xbar control chart was developed to measure the daily averages to show the improvement achieved in process and also post-project to ensure the results continued.
Step 2: Root cause analysis: 5 Whys
Waiting time depends upon the interactions among four factors:
- Daily load and the hourly arrival pattern of patients
- Processing speed (For example, if taking one blood sample takes three minutes then one technician can handle 20 patients/hour. If there are more than 20 arrivals per hour, a queue will develop.)
- Processing method (For example, batch or flow. Doctors are accustomed to signing test reports in batches toward the end of a rush period. This causes delays and lines for patients when they are trying to collect their test reports.)
- Deployment pattern of resources – employees and equipment (For example, a blood sample takes three minutes. If for two hours, patient arrivals peak at 30 per hour and only one technician is taking blood samples, a queue will develop even if the daily average of arrivals is 20.)
The process was measured to determine root causes of queue formation. Two parameters in particular were examined:
- Total load (all patients during the examined timeframe) was determined to average 300 patients per day (with a measured maximum of 350).
- Arrival patterns were mapped for a week and are shown in Figure 1.
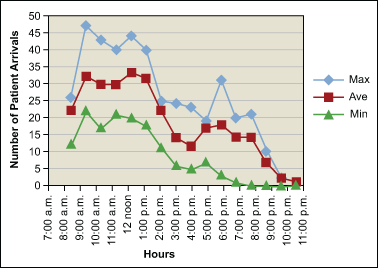
For the 16-hour period of operation each day, the peak hours were between 9 a.m. and 1 p.m. The average peak load was about 35 per hour, while the maximum hourly loads on some days in the week were 40 to 45 per hour.
Since the clinic does different types of tests (e.g., blood, urine, ultrasound, etc.) for which the equipment and personnel are not interchangeable, it was important to learn the workload of each category. This is shown in the pareto chart in Figure 2.
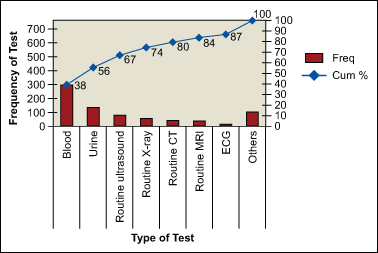
Viewed by departments, the data showed that the laboratory (blood and urine) accounted for 56 percent of the traffic, with routine ultrasounds and X-rays accounting for another 18 percent.
Additionally, all incoming patients had to register, be billed and pay at the reception area prior to departure. Thus, the reception area saw the maximum traffic.
Improvement was achieved in the two areas with the highest traffic: the laboratory (which represented the two highest frequency tests on the pareto chart, blood and urine) and reception.
Laboratory
As the lab was located on Floor 3, WIP mapping and a corresponding Xbar control chart began there.
In the current state, laboratory WIP was calculated as:
- Average = 14
- Average + 3σ = 31
The value-adding process – taking a blood sample – was timed to take an average of three minutes per patient. With the available resource of two technicians in a shift (during peak hours), 40 patients per hour should be able to be seen with little or no queuing. Data indicated that patient loads greater than 40 occurred on only three occasions (for one hour only per occasion) in a week.
Why then was a queue developing? Examination of hourly queue sizes over several days (Figure 3) showed that the queue developed during the first hour after opening, then remained constant or reduced gradually.
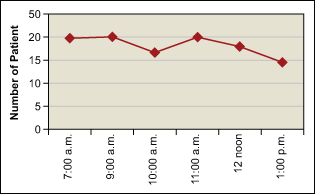
This meant that incoming loads and processing was proceeding apace between the peak hours of 9 a.m. and 1 p.m. The queue was forming in the off-peak hour of 7 a.m. to 8 a.m. and not decreasing until the peak time was over.
The start-up routine of the lab was examined. The center opened at 7 a.m.; one technician started work at 7 a.m. and calibrated the machines by 8:30 a.m. Sample taking began at 8:30 a.m. when the second technician reported for work. By this time the queue had already developed.
Steps 3 and 4: Countermeasures
A countermeasure was attempted – advancing the start time of one technician to 6:00 a.m.
Step 5: Check the result
A dramatic 50 percent reduction in laboratory WIP occurred:
|
Laboratory WIP |
Before |
After |
|
Average |
14 |
7 |
|
Average + 3σ |
31 |
15 |
The team was enthused by these results and immediately felt less pressure due to less WIP and fewer irritated patients. It was time to move to the next stage of the process.
After the change, WIP was low until 9 a.m., but a peak was building from 10 a.m. to 11 a.m.
Diabetic patients requiring post-meal blood tests who were at the lab at 8 a.m. returned two hours later at 10 a.m. after eating breakfast. When these patients were added to the queue of new patients, the load increased beyond 40 per hour, leading to a high WIP.
Steps 3 and 4: Countermeasures
A third technician was deployed for three hours – from 10 a.m. to 1 p.m.
Step 5: Check the result
The average laboratory WIP was further reduced by 30 percent as shown in the table below and the Xbar control chart in Figure 4.
|
Laboratory WIP |
Before |
After |
|
Average |
7 |
5 |
|
Average + 3σ |
11* |
9 |
* Between the time of the initial improvement of one additional attendant and the addition of the third staff member, the WIP reduced further from 15 to 11.
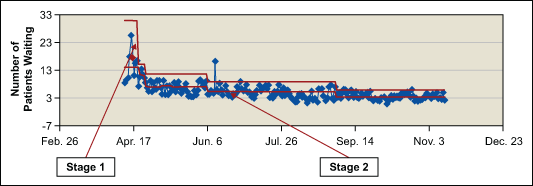
Reception
At the same time the changes to the lab were being implemented, the other major traffic area through which all customers passed – reception – was being improved.
Registration and billing were handled on the center’s ground floor, with registration being the first stop for all patients before they went for tests. CT and MRI tests were also on the ground floor. The combination required stopping points for patients at several times during a visit to the clinic. An analysis of WIP on the ground floor showed that 56 percent – a total of nine persons on average – were waiting in registration and billing lines. The registration process was measured to take three minutes per patient at each stage as shown in the table below .
|
Persons in Queue |
Waiting Time (Minutes) |
Average Waiting Time/Individual (Minutes) |
|
|
Registration |
5 |
15 |
3 |
|
Billing |
5 |
15 |
3 |
Since billing and registration were done sequentially (the patients paid before tests were run) on two counters, the patient was queuing twice for a total of 30 minutes in order to complete activities with a value-added time of only 6 minutes.
Steps 3 and 4: Countermeasures
A single-window billing and registration area would reduce the waiting time. The processing time was reduced from 6 minutes to 4.5 minutes per customer. With all three available counters performing billing and registration tasks, the peak arrival of about 40 visitors per hour (1.5 minutes per customer) meant the queuing time was reduced by more than 60 percent.
An additional problem observed in the reception area was that, like the lab (though to a lesser extent), a queue was building up by 8 a.m. This was easily addressed by having one reception counter open earlier – 6:30 a.m. instead of 7 a.m.
Step 5: Check the result
The percentage of the ground floor WIP comprised of registration and billing was reduced from 56 to only 20. Patients were now waiting mainly for MRI and CT availability.
The center’s control chart of ground floor WIP (Figure 5) reflects this improvement.
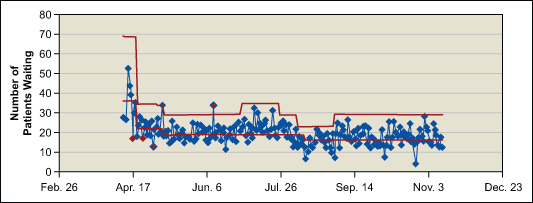
The weekly queues on the ground floor of the clinic were reduced by 50 percent.
|
Ground Floor WIP |
Before |
After |
|
Average |
37 |
17 |
|
Average + 3σ |
69 |
29 |
The queues for individual patients were reduced to 2 to 3 minutes at most times.
Steps 5 and 6: Check results and standardize results
The process was internalized quickly after the initial tests – employees felt less pressure as the customers were being serviced faster.
Step 7: Compile quality improvement story
The quality improvement story was prepared and presented to the company’s senior management team.
In addition to these improvements, a number of small Kaizens were held and achieved further successes. For example, a customer paid his bill and was due some change. He was asked to do the tests and come back as the required notes for his change were not available. When the patient was done with his tests, correct change was still not available. A simple change was required to prevent this type of problem from recurring. A system was introduced to provide the cashiers adequate change in the morning so they did not have to wait until cash was received from customers in the needed amounts.