
The nuclear medicine department located in the Ospedale Santa Croce e Carle in Cuneo, Italy, has always been recognized as a national and international reference site for its clinical compentencies and innovative facility design.
When originally opened, the nuclear medicine department was structured to provide the best possible service to patients. This included a focus on state of the art equipment, the latest clinical protocols and diverse professional compentencies of its staff. Today this department is still working hard to deliver excellent service to patients, at the same time being concerned about staff satisfaction and facing new challenges like, for instance, budget constraints.
Opening the Door to a Six Sigma Project
From the beginning of a Six Sigma continuous improvement, the key stakeholders were driven by an open-minded approach to sharing the department problems and issues, in order to benefit the department as much as possible.
In computed tomography (CT) or magnetic resonance imaging (MRI) modalities, patients rely on equipment to obtain diagnostic images. In functional imaging, however, patients are injected with a radioactive pharmaceutical and the patients themselves emit rays, which are detected by gamma camera or a positron emission tomography (PET) system, according to the energy window of the radioactive drug used for the clinical investigation needed.
In almost all types of exams, from the time of the injection to image acquisition, it is necessary to wait some time in order to have the radiopharmaceutical fixed in the region of the patient’s body where the pathology is located. This uptake time is the fundamental element to be taken into account during daily and weekly scheduling for each kind of exam. Another important issue is the characteristic of the acquisition systems, considering that in this department there are four gamma cameras (three single-head, and one dual-head system) and one PET-CT scanner. On the whole, the number of exams performed yearly is about 20,000 (including 11,000 in vivo studies, 4,200 dual-energy x-ray absorptiometry (DEXA), 2,700 thyroid endoscopies and 2,800 PET-CT investigations) divided among inpatients (15 percent), outpatients (80 percent and emergency department patients (less than 5 percent).
From CTQs to the Define Phase
During the project kick-off meeting, the critical-to-quality elements (CTQs) came up clearly and the project focus was set on the evaluation of the nuclear medicine department activity and workflow, as well as the thyroid endoscopy. The PET-CT environment was kept out of the project scope as noted in the table below.
| In and Out of the Project | |
|
In Scope |
Out of Scope |
| Four Gamma Camera Activity | PET/CT and DEXA Personnel Activity |
| Standard Personnel Shift | Personnel Overtime |
| Inpatients, Outpatients and ED Patients | Nuclear Medicine External Activity (e.g., Operating Room) |
| Nuclear Medicine and Thyroid Endoscophy Activity | |
The application of Six Sigma methodology was well suited to addressing a long process cycle time (from exam booking to report delivery), and the need to track it in order to check where and why it was delayed.
Actually, the nuclear medicine department had already mapped the process workflow in a high level process map from exam booking until report delivery. This provided a headstart for the Six Sigma project. In addition, the department had other issues related to staff communication and patient satisfaction as well as a long waiting list for bone and cardiac exams (20 and 40 days).
Going to the Measure Phase
The project team began the data collection by setting up two separate forms – one for nuclear medicine department and one for endoscophy activities – to capture the timing of every single step of the processes from exam booking to report delivery date. This included the type of investigation, the camera used, the number of acquisitions executed, the waiting time in between the different steps, etc.
Both processes were divided in two parts – from exam booking to report delivery and patient wait time in the department. The wait time was defined as from administrative admission to the exit. The team wanted to study in detail which process steps plays a key factor (Figure 1), keeping into account for endoscophy, the parts in which the physician is in charge (Figure 2).
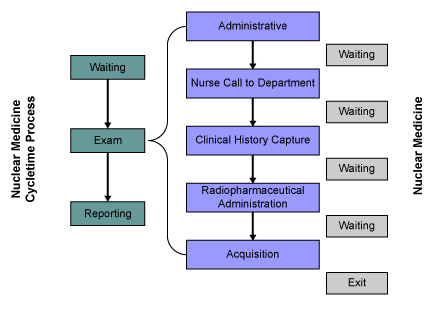
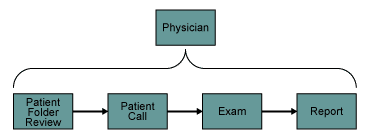
What the Project Team Analyzed
The data analysis pointed out some surprising situations, in other cases, problems were exactly as expected, such as the bottleneck for the clinical history capture. It had a long wait time (24 minutes) due to the fact that there was just one physician and one ward dedicated to this activity.
From the statistical analysis of the process cycle time, the waiting list for cardiac and bone exams turned out to be quite long as expected, 43 and 23 days for outpatients, although still within the local requirements (60 days).
As a matter of fact, the cardiologists’ availability for the nuclear medicine department activity was fixed and related to their activity in the cardiac department, but it represented the key to decreasing the waiting list, adding a weekly session and helping the department gain a competitive advantage over the hospitals located nearby.
The problem about the bone scan waiting list had been figured out when the project team analyzed the camera workload. The data was not consistant with the daily agenda as scheduled. For example, the whole body acquisition, which is one of the longest scan, had been performed from time to time with the single-head camera even though the dual-head one was available. It takes the single-head camera twice as long to scan.
According to the camera workload analysis, 40 percent of the acquisitions had been performed by the dual-head system, while the exam length and the downtime were too long for the single-head ones. This is where the idea to replace one of the single with a dual camera came from.
In addition to the suggestion of new equipment, these other ideas were raised during the project:
- An additional ward for the patient clinical history capture.
- A dual-head camera room.
- A physician reporting room.
- Minimize the patient path, keeping the attention on the radioprotection issue.
As the team considered physical changes in the department, it used a spaghetti chart, a Lean tool, to help in redesigning the layout.
From Analysis to Improvement
The opportunity to have a reporting room could solve a workflow problem raised by the data analysis: The patient length of staying in the gamma camera room compared to the acquisition length was too long. This was because, after the acquisition, the technologist had to look for a physician to see if there was any need for further investigations. This left the patient in the acquisition room and delaying the schedule.
In the analysis of endoscopy activities, the data showed the process cycle time was extremely long with excessive variability – an average of 50 days with a standard deviation of 36 days. Statistical analysis indicated three different sub-processes for inpatients, outpatients and patients with a check-up fixed from 60 to 90 days (70 percent out of the total exams). This fact explained the process cycle time length.
Another big issue was related to the fact that at least 15 percent of scheduled outpatient appointments did not present themselves at the endoscopy exam. The reason was the unacceptable waiting list of 15 days. This was considered by patients as too long compared to the same investigation done in private centers.
The project team checked the feasibility and suggested adding a patient in the daily agenda in order to shorten the waiting list and become more competitive.
Conclusion: 30 Percent Less Waiting
Overall, the Six Sigma project helped the nuclear medicine team to better understand and uncover some of the issues it has been facing in the routine workflow management. The project ultimately led to a 30 percent reduction in patient waiting time and an increase of the equipment utilization rate, while maintaining staff and patient satisfation.